


Alphadopa Tablet
Written By Dr. Swati Mishra, BDS,
Reviewed By Dr. Sachin Gupta, MD Pharmacology, MBBS,
Last updated on 20 Jan 2026 | 04:47 PM (IST)
Save more with additional offers








General Information

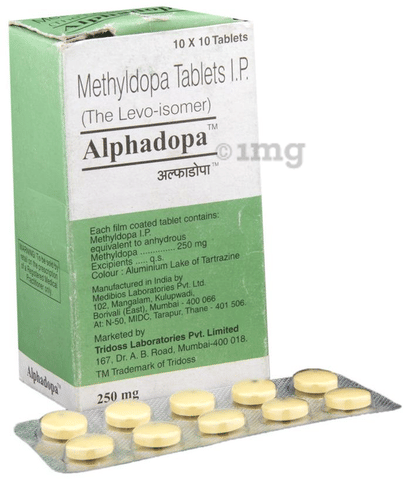



Product introduction
Alphadopa Tablet can be taken alone or in combination with other medicines. It can be taken with or without food. You may take it at any time of day but try to take it at the same time each day. You should take this medicine as advised by the doctor and never stop it abruptly without consulting the doctor. Most people with high blood pressure do not feel ill, but if you stop taking this medicine, your condition could get worse. This may lead to your blood pressure rising up again and increase your risk of heart disease and stroke.
It is important to have your blood pressure checked regularly. This medicine is only one part of a treatment program which should also include a healthy diet, regular exercise, smoking cessation, moderation of alcohol intake and weight reduction. You can eat normally while taking this medicine, but try to reduce your salt intake.
Common side effects of this medicine include headache, weakness, dizziness, and dryness in the mouth. Consult your doctor if these side effects bother you.
Before taking this medicine, it is better to let your doctor know if you are suffering from any kidney or liver disease. Also, pregnant women and breastfeeding mothers should consult a doctor before taking it. You must inform the doctor about all the other medicines that you are taking apart from this medicine.
Uses of Alphadopa Tablet
Benefits of Alphadopa Tablet
Hypertension, or high blood pressure, is a condition in which the force of the blood against artery walls is consistently too high, increasing the risk of heart disease, stroke, and kidney problems. Alphadopa Tablet is used to manage high blood pressure by helping to lower and stabilize it over time. Keeping blood pressure within a healthier range reduces strain on the heart and arteries, thereby helping prevent serious cardiovascular complications and improving overall well-being.
Side effects of Alphadopa Tablet
- Dizziness
- Fatigue
- Dryness in mouth
- Headache
How to use Alphadopa Tablet
Avoid Alphadopa Tablet with high protein meals such as cottage cheese, Swiss cheese, protein powder, eggs and milk.
How Alphadopa Tablet works
Quick tips
- For best results, take Alphadopa Tablet at the same time every day. Take last dose of the day at bedtime.
- May cause dizziness and lightheadedness. If this happens to you, do not drive or use machinery.
- Your doctor may monitor liver function. Inform your doctor if you notice yellowing of the skin or whites of the eyes, abdominal pain, nausea and vomiting while taking this medicine.
- Inform your doctor if you are pregnant, planning pregnancy or breastfeeding.
- Do not discontinue use without consulting your doctor even if you feel better.
- Dizziness or fainting may occur, especially when rising from a lying or sitting position. Getting up slowly may help improve the problem.
- Eat healthy (low-fat, high-fibre, low-sodium diet), quit smoking, limit alcohol intake, increase your physical activity, watch your weight, and reduce stress.
- Inform your doctor if you are pregnant, planning pregnancy or breastfeeding.
Safety advice

Alcohol

Pregnancy

Breast feeding

Driving
Kidney
Regular blood pressure monitoring is recommended for dose adjustment.

Liver
Interaction with drugs
Tranylcypromine (Oral Route)
Baclofen (Oral Route)
Methylphenidate (Oral Route)
Lithium carbonate (Oral Route)
Bortezomib (Injection Route)
Fact Box
Chemical Class
Habit Forming
Therapeutic Class
Action Class
Related lab tests
References
- Michel T, Hoffman BB. Treatment of Myocardial Ischemia and Hypertension. In: Brunton LL, Chabner BA, Knollmann BC, editors. Goodman & Gilman’s: The Pharmacological Basis of Therapeutics. 12th ed. New York, New York: McGraw-Hill Medical; 2011. pp. 773-74.
- Benowitz NL. Antihypertensive Agents. In: Katzung BG, Masters SB, Trevor AJ, editors. Basic and Clinical Pharmacology. 11th ed. New Delhi, India: Tata McGraw Hill Education Private Limited; 2009. p. 173.
- Briggs GG, Freeman RK, editors. A Reference Guide to Fetal and Neonatal Risk: Drugs in Pregnancy and Lactation. 10th ed. Philadelphia, PA: Wolters Kluwer Health; 2015. p. 894.
- Chaves RG, Lamounier JA. Breastfeeding and maternal medications. J Pediatr (Rio J). 2004;80(5 Suppl):S189-S198. [Accessed 19 Mar. 2019] (online) Available from:




User feedback
Want to know more
We provide you with authentic, trustworthy and relevant informationHave issue with the content
Disclaimer
Marketer details
Address: Wockhardt Towers, Bandra Kurla Complex, Bandra (East), Mumbai 400051, Maharashtra, India
Vendor Details
Lab tests offered by us
- CBC (Complete Blood Count)
- FBS (Fasting Blood Sugar)
- Thyroid Profile Total (T3, T4 & TSH)
- HbA1c (Glycosylated Hemoglobin)
- PPBS (Postprandial Blood Sugar)
- Lipid Profile
- Vitamin D (25-Hydroxy)
- Urine R/M (Urine Routine & Microscopy)
- Coronavirus Covid -19 test- RT PCR
- LFT (Liver Function Test)
- KFT (Kidney Function Test)
- TSH (Thyroid Stimulating Hormone) Ultrasensitive
- ESR (Erythrocyte Sedimentation Rate)
- Uric Acid, Serum
- Vitamin B12
- CRP (C-Reactive Protein), Quantitative
- Urine C/S (Urine Culture and Sensitivity)
- Serum Electrolytes
- Serum Calcium
- Serum Creatinine
- Diabetes Screening (HbA1C & Fasting Sugar)
- KFT with Electrolytes (Kidney Function Test with Electrolytes)
- Cholesterol - Total
- Hb (Hemoglobin)
- Complete Hemogram (CBC & ESR)