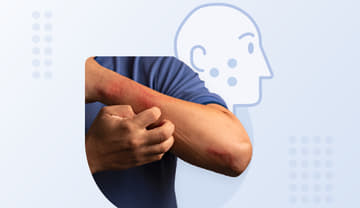
Eczema
Eczema is a common chronic skin condition characterized by dry, intensely itchy, and inflamed patches of skin. It originates from the Greek word ‘ekzein’ which means to ‘boil over’ or ‘break out’. Although there are several types of eczema, the term usually refers to the most prevalent form, called ‘atopic dermatitis’.
Atopic dermatitis results from a complex interplay between environmental and genetic factors. The word "atopic" in atopic dermatitis indicates an association with allergies. Though the condition is not always directly caused by an allergic reaction, it is commonly associated with other allergic conditions like asthma and hay fever.
The condition begins as lesions that are intensely red, bumpy patches or plaques that may ooze fluid when scratched. In chronic eczema, scratching and rubbing create skin lesions that appear scaly, dry, thicker, darker and scarred. While eczema is not contagious, the secondary skin infections associated with the condition may be.
Eczema can be lifelong and patients often cycle through long periods of symptom-free remission, followed by brief flare-ups that can be severe. However, symptoms can be prevented and managed with home care and remedies by keeping the skin healthy and moisturized. Exacerbation of eczema requires treatment in the form of corticosteroid creams. In addition to topical treatment, severe acute or chronic eczema often requires systemic immunosuppressant drugs or phototherapy.



