Want to know more?
Read Our Editorial PolicyHave issue with the content?
Report Problem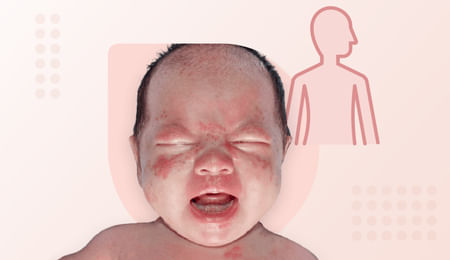
Urticaria
Also known as Hives, Welts, Weals and Nettle rashOverview
Urticaria is a condition characterized by itchy skin, reddened areas with defined borders, and swelling of the skin. It can be classified as acute or chronic based on the duration. Acute urticaria usually stays for 6 weeks while chronic urticaria may stay over 6 weeks. In most cases, chronic urticaria can recur frequently over weeks and months.
The most common causes of acute urticaria are allergic reactions to food, medicine, cosmetics or soap, infections, insect bites or stings, environmental pollutants, latex, extreme temperatures, emotional stress, and exercise. The cause of chronic urticaria is often difficult to identify and many times, impossible. However, in some cases, chronic urticaria can be linked to the conditions affecting the immune system or to diseases like hepatitis or cancer.
Urticaria can be mistaken for other skin conditions with similar appearance. However, a dermatologist can help to differentiate and diagnose the condition based on the symptoms, medical history and skin examination.
Urticaria can be prevented by avoiding exposure to any known causes, triggers or allergens. There is no specific treatment for urticaria as in most cases, the symptoms usually subside within a few days. In some cases, use of home remedies can help improve the symptoms like pain, swelling, and itching. If hives are caused by an allergy, then use of antihistamines might be advised. These are medications that counter the immune system’s chemicals released against the allergy.
Key Facts
- Children below 10 years of age
- Adults between 20 to 40 years of age
- Both men and women
- Skin
- Blood
- Hair
- Allergic contact dermatitis
- Urticarial vasculitis
- Drug eruptions
- Erythema multiforme
- Henoch-Schonlein purpura (IgA vasculitis)
- Mastocytosis
- Physical examination
- Allergy test
- Blood tests: Complete blood count (CBC), Erythrocyte sedimentation rate (ESR) & Antinuclear antibody (ANA)
- Angioedema tests
- Solar hives (urticaria) test: Photo testing & Patch testing
- Cholinergic hives tests
- Other tests: Imaging studies & Punch biopsy
- Antihistamines: Chlorpheniramine Maleate, Loratadine, Desloratadine & Cimetidine
- Anti-inflammatory medications: Prednisone
- Corticosteroids
- Immune suppressing medications
- Dermatologist
- Rheumatologist
- Immunologist
- Internist
- Allergist
- Pediatrician
Symptoms Of Urticaria
Urticaria, also known as hives, typically manifests as red or skin-colored lumps or welts with distinct borders. They can be as small as a pen tip or as huge as a dinner plate. Pressing the center of a red hive can cause it to become white, this is known as blanching. They may appear as a single hive or as blotches or linked patches. It appears to help in regulating the body's allergic reaction to certain stimuli.
It is common for people to mistake hives for other conditions, but they are distinguished by a few characteristics. You can determine whether hives are causing a rash or skin disease based on how long they last and how much they move. The following symptoms are commonly associated with hives.
-
Red or skin-colored lumps or welts with distinct borders that usually disappear within 24 hours but may return to another location.
-
Bumps or welts that appear alone or in clusters, covering a greater area.
-
Itchiness and/or swelling in the area of the bumps or welts.
-
Pain or stinging may occur at the site of the pimples or welts.
Causes Of Urticaria
The disease's etiology might be caused by a variety of reasons. Factors that are frequently encountered include:
1. Medications
Urticaria can be caused by certain medicines such as:
-
Penicillin
-
Nonsteroidal anti-inflammatory drugs
-
Sulfonamides
-
Thiazide diuretics
-
Oral contraceptives
-
Angiotensin-converting enzyme inhibitors
-
Vitamins
-
Curare and its derivatives
-
Synthetic adrenocorticotropic hormone
-
Radiocontrast agents
Urticaria rashes may appear anywhere from 1–2 hours to 15 days after oral consumption of the medicine or drug. They appear faster when medicines are administered intravenously as compared to oral administration.
2. Foods
Foods that are common causes of urticaria include:
-
Nuts
-
Eggs
-
Fish
-
Shellfish
-
Chocolate
-
Meat
-
Cow's milk
-
Fruits (citrus fruits, grapes, plums, pineapples, bananas, apples, and strawberries)
-
Vegetables (tomatoes, garlic, onions, peas, beans, and carrots)
-
Mushrooms
-
Fermented foods
-
Spices
-
Spirits
Note: Preservatives such as azo dyes, benzoic acid derivatives, salicylates, and food colors are also major causal factors. Urticaria generally appears 1–2 hours after intake of food. Children are more likely to develop food-related urticarial rashes.
3. Respiratory allergens
Urticaria can be induced by the inhalation of allergens like:
-
Pollen
-
Mold spores
-
Mites
-
Animal dandruff
-
Animal hairs
Note: Smoking is also a significant component since it includes numerous chemicals that might aggravate urticaria. Urticaria induced by respiratory allergens often develops shortly after contact.
4. Medical conditions
Urticaria can be caused by infections such as:
-
Tonsillitis
-
Dental abscesses
-
Hepatitis
-
Infectious mononucleosis
Note: Urticaria is caused by parasites, particularly in youngsters.
5. Contact urticaria
Urticaria can be caused through contact with:
-
Latex
-
Cosmetics
-
Chemicals
6. Insect bites
Insect bites may also cause urticaria, particularly in children.
7. Psychogenic factors
Stress, sorrow, and despair can worsen pre-existing urticaria as well as cause it.
8. Systemic disorders
Systemic disorders, in particular, can induce persistent urticaria. Thyroid and rheumatic disorders such as systemic lupus erythematosus, lymphoma, leukemia, and carcinomas may be examined if necessary. It should be mentioned that urticaria can arise during pregnancy.
9. External stimuli
Stimuli like pressure, heat, cold, and dermographism can all cause urticaria. Urticaria caused by pressure usually appears 3-4 hours after exposure. As a result, they are known as delayed pressure urticaria.
10. Hereditary urticaria
Urticaria can be hereditary and manifest in forms such as angioedema and familial cold urticaria.
11. Idiopathic urticaria
Sometimes, urticaria may occur because of unrecognized causes.
Skin allergies can be caused due to various factors that range from changes in weather to exposure to environmental toxins. Let us understand some of the common causes of skin allergies in children.
Risk Factors For Urticaria
Any of the following factors can raise the risk of acute or chronic hives.
-
Allergic reactions (whether pre-existing or newly developed).
-
A personal history of hives.
-
A history of hives in the family (especially in the case of hereditary angioedema, although rare).
-
A well-known condition related to hives (infections such as urinary tract infection, strep throat, hepatitis, rheumatoid arthritis, or type 1 diabetes).
-
Viral infections.
-
Medications (include codeine, aspirin, morphine, and NSAIDs).
-
Skin sensitivity or dermatitis (inflammation of the skin).
-
Sensitivities to disinfectants, colors, chemicals, or perfume scents.
-
Emotional triggers (association with stress and anxiety).
Allergies are caused when the body’s immune system responds abnormally to an external trigger known as ‘allergen’. Here’s everything you need to know about allergies.
Diagnosis Of Urticaria
Urticaria can be diagnosed by a variety of medical specialists, although family doctors make the majority of diagnoses (general practitioners).
Physical examination
A dermatologist diagnoses hives through a physical examination. However, in general, no particular tests are available to diagnose hives. This is due to the non-specific or idiopathic character of triggers in many cases. In certain situations, a trigger – such as a kind of medicine – can be discovered. If an outbreak of hives clears after discontinuing the drug, it can be determined whether it is a trigger. If it does not, the medicine is not the likely culprit.
A doctor will gather full medical history and perform a symptom discussion during the appointment in order to try to establish an underlying cause of hives, such as an allergic response, followed by a thorough physical examination.
The questions a doctor may ask during a consultation are:
-
How long have the symptoms been present?
-
How did the skin marks seem when they initially appeared?
-
Have the marks altered in any way (for example, size or form) since then?
-
Is there anything that has made your symptoms better or worse before your consultation?
-
Do the skin blemishes irritate, burn, or sting?
-
Before this consultation, have any markings vanished without leaving another trace, such as a bruise?
-
Have you been tested for allergies? If so, which?
-
Has a similar skin issue ever developed or happened before?
-
Have you tried any new meals for the first time?
-
Have any new goods been launched for the first time such as cleaning detergents?
-
Have you been bitten or stung by an insect lately?
-
Are you presently taking any new drugs (prescription or over-the-counter, including herbal supplements)?
-
Has a new pet been brought into the house?
-
Is there anyone in your family who has had a similar sort of skin problem?
Allergy test
The doctor will then do a physical examination and assess the skin marks (those that are present). If allergies are suspected, a skin prick test to detect the chemical causing the response may be done. The trigger may be very easily identified if urticarial rashes occur within a short period after intake of shellfish or peanuts, or exposure to sunshine or water, after a scrape to the skin, or after vigorous activity.
Once a trigger allergen has been identified, the doctor will advise avoiding coming into contact with or eating a specific food, as well as other items produced from or containing the chemical. If judged safe, the doctor may prescribe an oral food/drug test, in which the afflicted individual is asked to the suspected allergen (in a defined amount) in order to elicit a hive reaction. The patient is monitored closely throughout the test, with emergency equipment or medicine on standby. If there are significant chances of serious responses, such as anaphylaxis, these tests may not be conducted.
If you experience any symptoms of allergy, get an allergy panel done.
Blood tests
Blood tests may also be advised to screen for certain diseases known to be related to hive outbreaks and to analyze blood proteins for a possible genetic tendency (as in the case of hereditary angioedema). A urine sample is occasionally collected as well.
Note: Laboratory studies generally are not indicated for acute urticaria (< 6 weeks).
In the event of chronic hives, the following tests may be advised as applicable:
-
Complete blood count (CBC) to check for signs of anemia or any infections.
-
Thyroid function test to determine if the thyroid is hyperactive or underactive (hyperthyroidism or hypothyroidism).
-
Tests for liver function to look for any underlying liver condition.
-
Erythrocyte sedimentation rate (ESR) test is used to determine the rate of erythrocyte sedimentation (to assess any immune system abnormalities).
-
Stool test to assess for or identify any parasites causing an infection
-
Antinuclear antibody (ANA) test to rule out autoimmune disorders such as lupus.
Angioedema tests
C1 esterase inhibitor test (this test evaluates complement protein levels and helps detect any underlying causes of edema) and complement components (C2 and C4) to screen for deficits. Low amounts of these components might cause symptoms of edema and inflammation in the body.
Solar hives (urticaria) test
Photo-testing: A doctor or allergist can evaluate skin responses to UV radiation from a sun lamp using a range of wavelengths. The wavelength to which the skin reacts will be utilized to identify the type of solar allergy.
Patch testing: It involves applying certain chemicals (a suspected sensitizer agent that may cause a response) to the skin and covering it with a patch or dressing for a period of time (usually 24 to 48 hours). The region will next be examined to determine the likelihood of a response. After that, the skin may be exposed to UV light (radiation) via a sun lamp. If the skin responds, solar hives can be diagnosed.
In symptoms, autoimmune or metabolic signals may be checked by blood samples (and occasionally skin biopsies) to establish an underlying cause.
Cholinergic hives tests
-
An exercise challenge test: The patient may be asked to complete an exercise program in order to elicit a comparable response. During the challenge, medical devices may also be used to obtain various measures.
-
A passive warming test: During the exposure test, a doctor would use warm water or increased ambient temperature to elevate the patient's internal body temperature and monitor a probable reaction.
-
A skin test for methacholine: Methacholine, a non-selective muscarinic receptor, would be administered to activate the parasympathetic nervous system and monitor a potential response.
Other tests
Other studies that may be considered include the following:
-
Imaging studies: These are generally not indicated unless suggested by a specific symptom or sign.
-
Punch biopsy: It is advised if urticarial vasculitis (inflammation of blood vessels) is suspected.
Extensive testing is not generally recommended by medical specialists in the event of minor hive breakouts or a single incident. Chronic hives are seldom associated with an allergic reaction (due to the frequency of recurrences, which can last for more than 6 weeks). It is more likely that the reason is not of external origin. Relevant tests are performed to identify an underlying cause, which might be an autoimmune illness or another medical condition.
Celebs affected
Prevention Of Urticaria
Making lifestyle changes that minimize or prevent hive flare-ups is generally the most effective strategy to lessen the chance of an outbreak or recurrence. It is not always possible to entirely avoid a hive breakout. A confirmed allergy (or a known cause such as medicines, environmental factors, foods, or exposure to specific pets) is a one-way trigger that can be easily avoided. Specific allergy treatment can also be used to minimize the risk and relieve breakouts.
If the reason is unknown and flare-ups occur often, maintaining a record that draws parallels between ‘cause and effect' (e.g., food ingested and a probable response) might help discover and avoid potential triggers.
-
Careful management of sun exposure (refraining from being out in the sun when it is at its strongest – often between 10 am and 4 pm, and gradually increasing time outdoors during the in-between months – spring and autumn or fall – to try and better adapt to stronger sunlight exposure) can be beneficial for solar hives.
-
Wearing lightweight or loose woven clothes that give maximum covering (long pants or skirts as well as sleeved items).
-
Wearing clothes with a UPF (ultraviolet) protection rating of at least 40, as well as a broad-spectrum sunscreen recommended by the treating medical professional (and applied regularly).
-
Maintain your calm. Hives can be triggered by stress. If you are frequently stressed, practice effective stress-reduction strategies including daily exercise, meditation, and mindfulness.
-
Certain products that may irritate the skin should be avoided. When you have hives, some soaps might cause your skin to dry out and create greater irritation. Make sure you use a mild soap designed for delicate skin. There are many to choose from here. These are generally free of scent and other irritants. You should also avoid using irritants such as heavy moisturizers and creams. When in doubt, use a solution that is designed for sensitive skin. Applying it shortly after washing may also help with itching.
-
Using anti-sun aids such as sunglasses, broad-brimmed hats, and umbrellas can help to protect against sun rays.
Specialist To Visit
The symptoms of urticaria are often easy to manage with the use of over-the-counter medications and lifestyle changes. However, if you experience rashes and itchy skin that seem different or worse than usual, consult a doctor. Also, if you experience these symptoms for more than 6 weeks or on a regular basis, immediately visit your doctor’s clinic to know the exact cause and get it treated.
Specialists that can help to manage urticaria include:
-
Dermatologist
-
Rheumatologist
-
Immunologist
-
Internist
-
Allergist
-
Pediatrician (for children)
Getting the right diagnosis and the right treatment can help in better prognosis and improve the quality of life. Consult the best experts online.
Treatment Of Urticaria
If your symptoms are minor, you might not require therapy. Hives and angioedema often resolve on their own. However, therapy can provide relief for severe itching, severe discomfort, or symptoms that linger.
Medications
Prescription medicines, such as those listed below, may be used to treat hives and angioedema.
Anti-itch medications (antihistamines)
Some class H1 antihistamines with drowsiness as a side effect are:
-
Chlorpheniramine
Examples of non-sedating second-generation H1 antihistamines are:
Second generation H1 antihistamines include:
Examples of H2 antihistamines:
Treatment usually begins with a non-sedating antihistamine during the day and a sedating antihistamine at night. All antihistamines are equally effective in the licensed dosage. If patients do not respond to standard dosage, it is common to double or triple the dose of non-sedating antihistamines.
If patients complain of indigestion or acidity, H2 antihistamines might be administered. Combination therapy is frequently beneficial to the patient. In a short experiment, fexofenadine outperformed generic levocetirizine. Many patients do not react to these combinations, necessitating the use of second-line treatments. According to some research, 40% of patients did not respond to antihistamines.
Anti-inflammatory medications
Doctors may occasionally give an oral corticosteroid medication such as prednisone to decrease swelling, redness, and itching caused by severe hives or angioedema.
Immune suppressing medications
If antihistamines and corticosteroids do not work, your doctor may prescribe immune suppressing medication that might calm a hyperactive immune system.
Situations of emergency
Acute urticaria may progress to life-threatening angioedema and/or anaphylactic shock in a very short period, although anaphylaxis usually presents as rapid-onset shock with no urticaria or angioedema.
A trip to the emergency department and an emergency injection of epinephrine — a kind of adrenaline — may be required if you have a severe episode of hives or angioedema. If you have had a major attack or if your attacks continue after therapy, your doctor may advise you to carry a pen-like device that allows you to self-inject epinephrine in an emergency.
If associated bronchospasm is present, prehospital nebulized albuterol may be warranted.
Other measures may be appropriate, such as continuous ECG, blood pressure and pulse oximetry monitoring, administering intravenous crystalloids if the patient is hypotensive and administering oxygen.
Home-care For Urticaria
If someone has minor hives or angioedema, the following methods may help ease their symptoms.
-
People should stay away from triggers and take appropriate precautions. Foods, medicines, pollen, pet dander, latex, and insect bites are the most common triggers. If you suspect a medicine for your rash, discontinue its use and notify the primary care practitioner.
-
Over-the-counter itch relievers help reduce itching. Some non-prescription antihistamines are loratadine, cetirizine & diphenhydramine.
-
You can apply a cool washcloth to the affected region to soothe the irritated skin. It also helps avoid scratching.
-
A relaxing bath in cold water or a cold shower might provide relief from itching. Some people may benefit from bathing in cool water sprinkled with baking soda or oatmeal powder, but this is not a long-term option for chronic itching management.
-
Dressing in loose-fitting, smooth-textured cotton will help avoid skin irritation.
-
Staying out of the sun and seeking shade when outside will help prevent aggravation of painful rashes and itching.
Complications Of Urticaria
Urticaria may lead to anaphylaxis. Anaphylaxis is one of the most serious complications of hives. It is an allergic reaction that is often severe and may even be fatal. It usually happens within seconds to minutes of exposure to a potential allergen such as peanuts or bee stings.
An anaphylactic reaction is produced due to a serial release of chemicals by the immune system, which might cause you to go into shock. Anaphylaxis is marked by rapid blood pressure drop and constriction of airways, preventing the sufferer from breathing.
The signs and symptoms of anaphylaxis are:
-
Fast and weak pulse
-
Skin rash
-
Nausea and vomiting
-
Swelling in the throat can cause a life-threatening obstruction of the airways
Certain foods, some medications, insect venom, and latex are common triggers for anaphylaxis.
Alternative Therapies For Urticaria
Home remedies for urticaria
1. Use a cold compress
The cold temperature of water or ice does wonders for soothing irritated skin. Simply soak a cloth or towel in cold water and apply to hive-affected areas of skin.
2. Make use of an oatmeal scrub
Oatmeal's anti-inflammatory properties make it an excellent hydrating and relaxing scrub for the skin. To soothe inflamed skin, take a lukewarm shower every morning and gently clean the areas of skin with hives infections with an oatmeal soap bar or scrub with baking soda.
3. Apply aloe vera gel
Aside from being a natural hydrator, aloe vera gel includes a large amount of beneficial antibacterial components. Applying a thick coating of aloe vera gel before bedtime significantly relieves the redness and discomfort associated with hives.
Ayurvedic treatment for urticaria
Follow these steps to cure urticaria rash with an ayurvedic treatment.
1. To minimize urticaria, take a 5 to 7 gramme dosage of a paste made from neem leaves, guduchi (giloy) leaves, or aloe vera pulp every day.
2. Take 1 teaspoon turmeric powder two to three times a day with a glass of milk or water. It's a fantastic remedy for boosting the body's immunity.
3. Massage the skin for 15 minutes with mustard oil before bathing in lukewarm water.
4. Mix 12 teaspoons black pepper (kali mirch) powder with 12 teaspoons desi ghee and eat it first thing in the morning on an empty stomach. For best effects, continue for up to three months.
Eczema, a form of skin inflammation, is commonly characterized by itchiness, red skin, small bumps and thickened skin over a period of time. Here’s more information about home remedies for eczema.
Living With Urticaria
Hives – itchy red or skin-colored welts, also known as urticaria – affect about 20% of the population. They are frequently the result of an allergic reaction to a meal or medication and usually dissipate soon.
Hives may be very itchy, as well as unpleasant. Although hives are clearly a physical burden, they can also be detrimental to emotional well-being, isolating individuals socially and hindering their performance at work or school, especially if they have suffered from hives for a long time.
However, for a tiny percentage of people, hives recur with no recognized cause. Chronic idiopathic urticaria (CIU) or chronic spontaneous urticaria (CSU) occurs when fresh outbreaks occur practically every day for 6 weeks or longer (CSU). It affects one percent or less of the population. People between the ages of 20 and 40 are the most likely to suffer from it. A single outbreak of CIU generally lasts no more than 24 hours. However, following that, additional colonies emerge.
Urticaria vs. contact dermatitis vs. insect bites
Although used interchangeably, these three terms have different meanings.
Hives (urticaria): These are itchy, red welts caused by an allergic response. The welts vary in size and emerge and disappear on a regular basis as the response progresses. Chronic hives occur when welts form for more than six weeks and repeatedly recur throughout months or years.
Contact dermatitis: Contact urticaria is characterized by an immediate but temporary localized swelling and redness on the skin upon direct contact with an offending chemical. Contact urticaria should be distinguished from contact dermatitis, which occurs hours to days after contact with the offending agent.
Insect bites: Bug bites may resemble hives in appearance, but hives behave differently. Hives can change shape and move around the body, whereas a bug bite remains in one spot. Rosacea often manifests as redness on the face, with enlarged blood vessels visible.
Urticaria in pregnancy
It is unlikely that chronic urticaria would flare up during pregnancy. Pruritic urticarial papules and plaques of pregnancy (PUPPP) and pemphigoid gestationis are special disease of the skin, especially one that does not cause inflammation in pregnancy, with urticaria-like lesions that appear during the second or third trimester of pregnancy and disappear after delivery. Sex hormones may have a role in illness pathophysiology.
Frequently Asked Questions
References
- Godse KV. Chronic urticaria and treatment options. Indian journal of dermatology. 2009 Oct;54(4):310.
- Kayiran MA, Akdeniz N. Diagnosis and treatment of urticaria in primary care. Northern clinics of Istanbul. 2019;6(1):93.
- Schaefer P. Acute and Chronic Urticaria: Evaluation and Treatment. Am Fam Physician. 2017 Jun 1;95(11):717-724.
- Kanani A, Betschel SD, Warrington R. Urticaria and angioedema. Allergy, Asthma & Clinical Immunology. 2018 Sep;14(2):1-3.
- Ring J, Brockow K, Ollert M, Engst R. Antihistamines in urticaria. Clin Exp Allergy. 1999 Mar;29 Suppl 1:31-7.