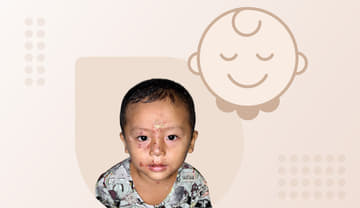
Impetigo
Impetigo is a contagious skin infection that mostly affects kids but adults can get it too. It is caused by bacteria, typically Staphylococcus aureus or Streptococcus pyogenes, entering through breaks in the skin like cuts, scratches, or insect bites.
While it can occur anywhere on the body, it often targets the face, hands, and feet. The main symptoms of impetigo are red sores or blisters that burst and form a honey-colored crust on the skin. Risk factors include
poor hygiene, crowded living conditions, and skin injuries, with children being more susceptible.
Treatment involves topical or oral antibiotics to eradicate the bacteria, along with proper hygiene practices. Although impetigo is usually a self-limiting condition, prompt intervention is essential to prevent its spread.



